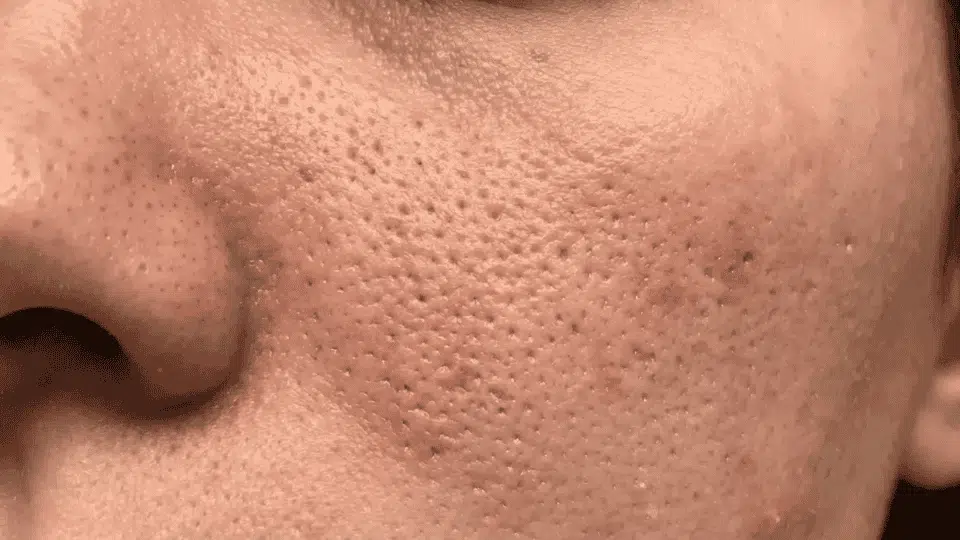
The bumpy, dimpled skin texture resembling the surface of an orange rind is known medically as peau d’orange, which means “skin of an orange” in French. It can appear on the face, breast, legs, or other parts of the body.
It’s important to understand that this texture isn’t always harmless; sometimes it’s just a cosmetic issue, but other times it may signal a medical concern requiring urgent evaluation, such as inflammatory breast cancer.
I’ll explain what this skin change looks like up close, its causes, from fluid retention to serious conditions, how it differs from cellulite, when to consult a doctor, and possible treatments based on the underlying reason. If your skin feels unusual lately, keep reading.
What is Orange Peel Skin?
Orange peel skin is a textured skin appearance that resembles the exterior of an orange, characterized by dimpling, thickening, and unevenness.
It occurs when connective tissue is pulled downward while fluid or swelling pushes upward, producing a pitted look. This condition can arise from cosmetic factors, blocked lymphatic drainage, or inflammation.
The term “peau d’orange,” meaning “skin of an orange” in French, describes this specific texture and is used medically.
It is not a standalone disease but a sign often observed in conditions such as lymphedema or breast cancer. Although its appearance doesn’t confirm cancer, it warrants further investigation to uncover the underlying cause.
For those whose orange peel texture appears on the face, it often connects back to how well the skin is being maintained daily, and following a consistent oily skin care plan can make a visible difference in overall skin texture over time.
When examining your skin, look for a dimpled surface with small indentations, tiny pits similar to an orange rind, thickened or swollen areas, redness or warmth, and a firm texture that feels tense and resistant.
Can Orange Peel Skin Go Away?
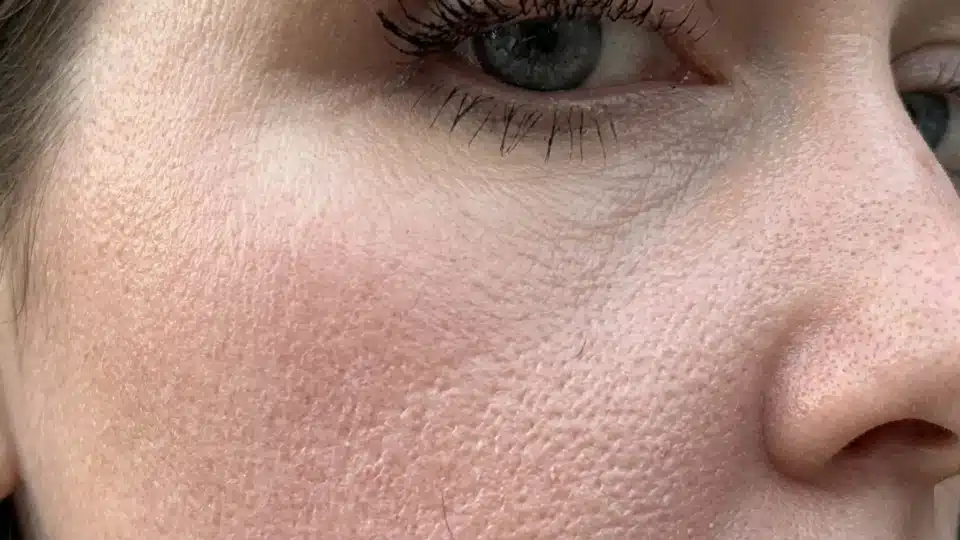

Whether this texture resolves depends entirely on the underlying cause. If it stems from temporary fluid retention or a treatable infection, the skin texture can improve significantly once the root issue is addressed.
In cases of lymphedema, consistent management, like compression therapy and drainage techniques, can reduce the appearance over time, though it may not disappear completely.
When the cause is more serious, such as inflammatory breast cancer, treatment focuses on the condition itself rather than the texture.
The skin change is a symptom, not the problem. Treating the source is what creates real change, so the answer is: sometimes yes, sometimes partially, and always condition-dependent.
Why Does Orange Peel Skin Appear?
This texture change usually occurs because of swelling, blocked lymphatic flow, or inflammation pushing against the skin’s connective tissue from beneath.
1. Aging, Sun Damage, or Loss of Skin Elasticity
Not all orange peel texture is caused by swelling. On the face, it is often linked to natural aging and reduced skin elasticity. As collagen and elastin decline over time, the skin loses firmness and support. This can make pores appear larger and create a slightly dimpled surface.
- Decreased collagen and elastin weaken the skin structure
- Sun damage accelerates loss of firmness and pore enlargement
- Most commonly seen on the face and not related to fluid buildup
2. Inflammatory Breast Cancer (Most Serious Cause)
Inflammatory breast cancer (IBC) is the most serious cause of peau d’orange and the one doctors act on fastest. Cancer cells block the lymph vessels within the skin of the breast, causing lymphatic fluid to back up.
This pressure forces the skin to dimple around the hair follicles, producing the orange peel effect. IBC doesn’t always form a distinct lump, which is why the skin change itself is a critical diagnostic clue.
- Cancer cells directly obstruct dermal lymphatic vessels, trapping fluid in the skin layers
- The texture appears rapidly, often over days or weeks, not months
- It frequently covers a large portion of the breast and is accompanied by redness or warmth
3. Lymphedema
Lymphedema occurs when the lymphatic system is damaged or blocked and can no longer drain fluid efficiently from the body tissues.
This fluid accumulates under the skin, stretching it and pulling at the follicles, which produces the pitted texture. It commonly follows cancer treatment, surgery, or an infection that damages lymph nodes.
- Damaged or removed lymph nodes reduce the body’s ability to circulate lymph fluid normally
- Chronic fluid buildup creates progressive skin thickening and firmness over affected areas
- The condition is manageable but rarely cures completely without consistent long-term care
4. Infection or Cellulitis
Cellulitis is a bacterial skin infection that causes deep inflammation in the skin and underlying tissue.
As the body responds to infection, the area becomes swollen, red, and warm, and the inflammatory pressure can produce a dimpled or orange-peel-like appearance, particularly on the legs.
- Bacterial invasion triggers an inflammatory response that swells tissue quickly and visibly
- The skin may appear stretched, shiny, and warm to the touch in the infected area
- Prompt antibiotic treatment usually resolves the texture as inflammation subsides
5. Fluid Retention or Severe Edema
Generalized fluid retention from heart conditions, kidney dysfunction, venous insufficiency, or prolonged immobility can cause enough localized swelling to create an orange-peel skin texture, especially in the lower limbs. The effect is typically less pronounced than that of lymphedema.
- Systemic conditions like heart or kidney disease can cause fluid to pool in limb tissues
- Prolonged standing, heat, or inactivity can trigger temporary but visible skin texture changes
- Addressing the underlying health condition typically reduces swelling and texture over time
Orange Peel Skin on the Breast?
When this texture appears on the breast, it usually isn’t the only sign. Watch for signs such as:
- Rapid swelling without clear injury
- Persistent redness covering a third of the breast
- Constant warmth unrelated to breastfeeding or infection
- Nipple inversion, flattening, or discharge
- Heaviness or fullness in one breast
Inflammatory breast cancer differs because it spreads through the skin’s lymph vessels rather than forming a lump. It often causes quick changes such as redness, warmth, swelling, and a peau d’orange texture.
IBC is more aggressive, tends to be diagnosed late, and requires different treatment. Since it can resemble an infection, any skin changes that do not improve should be evaluated by a doctor immediately.
When Should You See a Doctor?
See a doctor promptly if you notice any sudden changes in the texture or appearance of your breast skin, rapid thickening in any area, or pain accompanied by redness in the same spot.
Also seek medical attention if you have a fever along with swollen, red skin, or if your symptoms worsen within days rather than remaining stable. Do not wait to see if the condition “goes away” when breast skin is involved.
Treatment Depends on the Cause
Treatment consistently addresses the root cause of the condition, focusing on its fundamental factors rather than merely altering surface texture.
- Treating infection (cellulitis): Antibiotic therapy, oral or intravenous, depending on severity. Skin appearance typically improves as the infection clears.
- Managing lymphedema: Compression garments, manual lymphatic drainage, and skin care to prevent progression. Ongoing management is usually required long-term.
- Cancer treatment (IBC): Chemotherapy is typically the first step, followed by surgery and radiation. Treatment is aggressive, given IBC’s rapid progression.
- Managing fluid retention/edema: Address the underlying cause, heart, kidney, or vascular conditions, alongside compression and elevation where appropriate.
Texture improvement is possible in many cases, but outcomes depend entirely on how well the root condition responds to treatment.
Final Thoughts
Skin texture can tell a detailed story, and orange peel skin is one worth listening to. From manageable conditions like edema and cellulitis to serious diagnoses like inflammatory breast cancer, peau d’orange is a visible signal that something beneath the surface has changed.
This blog walked through the appearance, causes grouped by seriousness, the breast-specific concerns that deserve urgent attention, how it differs from cellulite, and what diagnosis and treatment actually look like.
Knowledge here isn’t meant to cause panic; it’s meant to prompt the right action at the right time. If something on your skin looks or feels unfamiliar, trust your instinct.
Have questions about what was covered? Drop them in the comments, or share this with someone who needs it.